The evidence for using cognitive behavioural therapies (CBT) and mindfulness-based interventions (MBIs) in management of migraine pain
Recent clinical practice guidelines and systematic reviews
The evidence for cognitive behavioural therapy (CBT) and mindfulness-based interventions (MBIs) for migraine pain
Behavioural, cognitive, and mindfulness-based therapies have an increasing evidence base for use as an intervention for management of chronic migraine pain. Below is a selection of a few recent clinical practice guidelines and systematic reviews related to the use of cognitive behavioural therapy and mindfulness-based therapies for management of migraine headache.
A selection of top-level evidence, including clinical practice guidelines (CPGs), systematic reviews, and RCTs, are provided below.
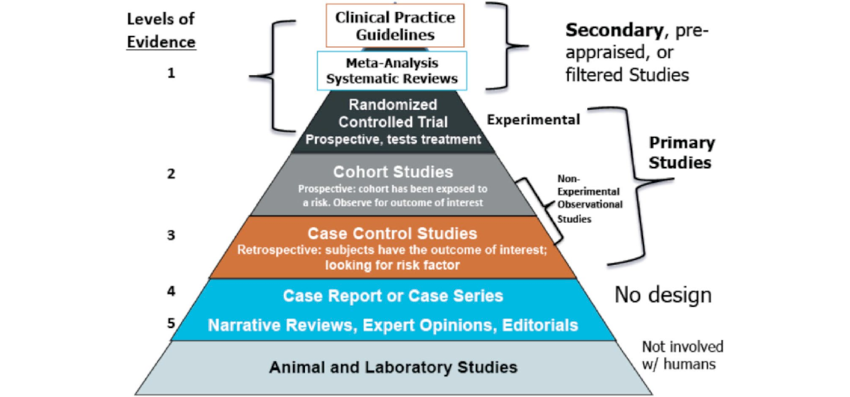
Clinical Practice Guidelines and Position Statements
International Headache Society Global Practice Recommendations for Preventive Pharmacological Treatment of Migraine (2024)
Behavioral interventions such as relaxation training, thermal biofeedback, electromyographic biofeedback, cognitive behavioral therapy, mindfulness-based therapy and acceptance and commitment therapy may be used alone or in combination with drug therapy to achieve improvement in migraine symptoms.
German Society for Neurology (Deutsche Gesellschaft für Neurologie - DGN) and the German Migraine and Headache Society (Deutsche Migräne- und Kopfschmerzgesellschaft - DMKG) - Treatment of migraine attacks and preventive treatment of migraine (2022)
Prevention treatment using medication should generally be accompanied by psychological procedures such as education, self-observation, self-management, cognitive behavioural treatment, social skills training, relaxation procedures, mindfulness, biofeedback and others. In patients with pronounced migraine-related impairment and/or psychological comorbidity, psychological pain treatment methods should always be used.
Mindfulness can be recommended for the preventive treatment of migraine in terms of improving quality of life.
The American Headache Society Consensus Statement: Update on integrating new migraine treatments into clinical practice (2021)
Biobehavioral therapies—specifically, cognitive behavioral therapy, biofeedback, and relaxation therapies—are effective in the preventive treatment of migraine, with Grade A evidence for their use as preventive therapies and limited evidence and clinical experience supporting their use as acute therapies. In addition, mindfulness-based therapies (e.g., mindfulness-based cognitive therapy, mindfulness-based stress reduction) and acceptance and commitment therapy are active topics of research and have a growing evidence base for use in migraine.
Systematic Reviews
Effects of mindfulness-based interventions (MBIs) on headache pain in migraine patients: A systematic review and meta-analysis. (2026)
MBIs have shown effectiveness in reducing headache pain in migraine patients. Clinicians and health professionals should consider utilizing MBIs as alternative or complementary treatments to reduce the severity of headaches in these patients.
Randomized Controlled Trials (RCTs)
Randomized controlled trial of neurofeedback mindfulness meditation as a practice for migraine management (2025)
The findings indicate that neurofeedback mindfulness meditation enhances headache management self-efficacy, yet larger trials are required to estimate effects with adequate precision. We discuss how improved self-agency may foster greater awareness and behavioural control over internal and external adjustments, ultimately leading to effective migraine recovery and prevention.
Mindfulness-Based Cognitive Therapy as Migraine Intervention: a Randomized Waitlist Controlled Trial (2022)
With respect to migraine parameters we did not find a significant group difference in the primary outcome (headache-related impairment), but the intervention resulted in a significant reduction of headache frequency (p = .04). In the analysis of secondary outcomes, MBCT showed superiority in four out of eight psychological parameters (perceived stress, anxiety, rumination, catastrophizing) with small to medium effect sizes. The intervention proved to be feasible and participants reported high degrees of contentment and achievement of personal goals.
Effectiveness of Mindfulness Meditation vs Headache Education for Adults With Migraine: A Randomized Clinical Trial (2021)
Mindfulness-based stress reduction did not improve migraine frequency more than headache education, as both groups had similar decreases; however, MBSR improved disability, quality of life, self-efficacy, pain catastrophizing, and depression out to 36 weeks, with decreased experimentally induced pain suggesting a potential shift in pain appraisal.
